Physiotherapy-approved Exercises to Relieve your Back Pain
Brace yourselves – this is going to be a long (but really informative!) one.
I’m Bernice, one of the physiotherapists here at Viva, qualified and trained in clinical Pilates and yoga teaching. I’ve encountered numerous close calls where I feel my back strain, when I don’t use good technique when working out, lifting or doing simple daily activities. I personally benefit every day from my physiotherapy, yoga and Pilates skills which I would love to share with you through this blog post to provide you with some knowledge around back pain.
Firstly, if you have come to this page with back pain, we would like to extend our deepest empathy to you as we understand how debilitating it can be. It has been stated that back pain can be more painful than even childbirth!
You are not alone, however. According to The American Association of Neurological Surgeons, an estimated 75-85% of people experience back pain at some point in their lives (Zalatimo, n.d.).
What to expect
Possible Sources of my Back Pain
Broadly, back pain can come from different types of mechanisms. There is mechanical/non-specific back pain, back pain that results from a structural damage,
Mechanical Back Pain
A large proportion of back pain is mechanical/non-specific – that means that there is no structural damage or pathology. Heavily backed by research, we know that exercise, in particular, strengthening the deep core in conjunction with the superficial core muscles, works best (Hayden et al., 2021).
Structural Back Pain
Without getting too technical, we have many structures that comprise your back.
We have vertebrae (many individual bones connected that comprise of your spine), muscles, tendons (tissues that connect muscles to bones) and ligaments (tissues that connect and reinforce the strength between adjacent bones/joints), discs (structures between your spinal vertebrae that act as shock absorbers), spinal cord (a thick rope of nerves that run through your spine) and nerves (that leave your spine between each adjacent vertebrae) (American Association of Neurological Surgeons, n.d.).
Back pain can happen when mechanical or structural problems develop in the discs, muscles, ligaments or nerves of the spine. This can happen slowly over time/degeneration, or due to an acute incident or injury.
Nerve injury
They are a major source of back pain. There are primary and secondary nerve pain.
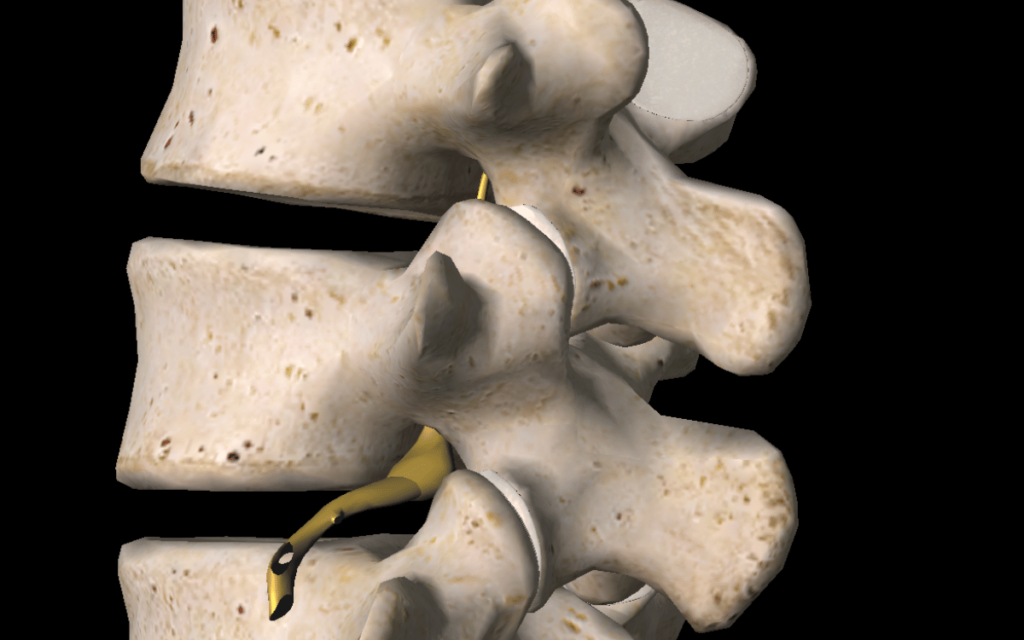
Primary nerve pain: originates from a disease/injury to the nerves in the brain, spinal cord or nerve roots (where the nerves exit your spine) e.g. nerve compression or trauma.
Secondary nerve pain: injury to the peripheral nerves that run outside of the spine i.e. down your arms or legs.
Image: Nerve Root (3D4Medical from Elsevier, 2023)
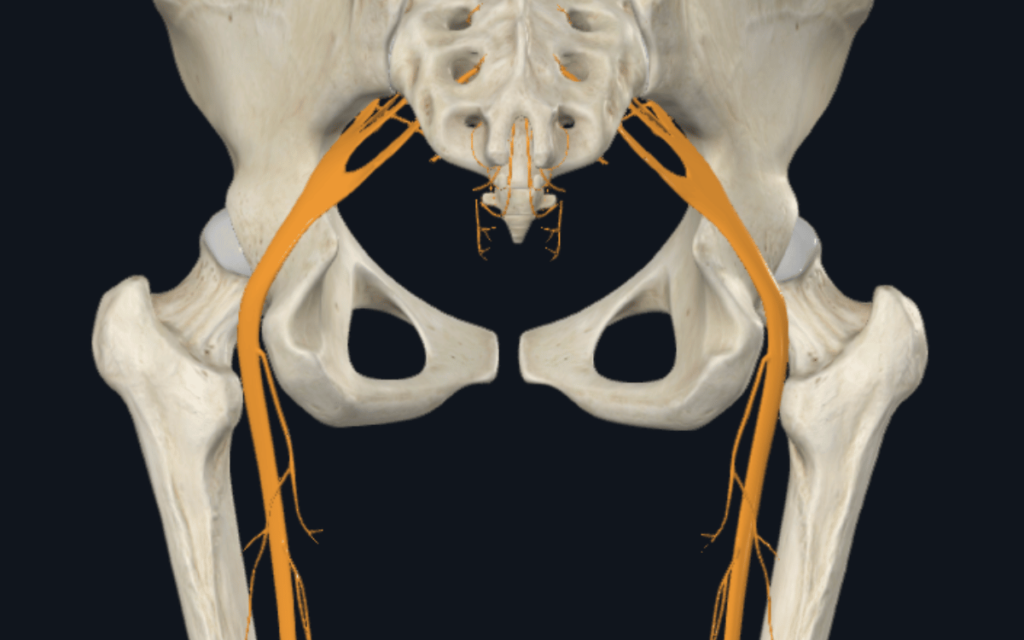
Due to the nature of nerves, when you get a nerve pain, you may feel it in your back, or anywhere else down the pathway of your nerve. The nerves that innervate your arms exit from your neck, forming a nerve network called the ‘brachial plexus’. One of the biggest ‘guilty’ guys is the sciatic nerve. After it exits your spine, it comes out through your pelvic bone, down your bum and branches out to many nerves to innervate your entire leg.
Image: Sciatic Nerves (3D4Medical from Elsevier, 2023)
When you get a nerve injury, your pain might be sharp or burning. It may also be associated with numbness and/or tingling pins and needles anywhere in the pathway of the nerve.
Sprain
An injury to the ligaments that support the spine – often occurring from twisting or lifting improperly. This happens more often if your deep spinal muscles are weak.
Strain
An injury to a muscle or tendon in your back.
Degenerative Disc
As you get older, the disc gets weaker and breaks down.
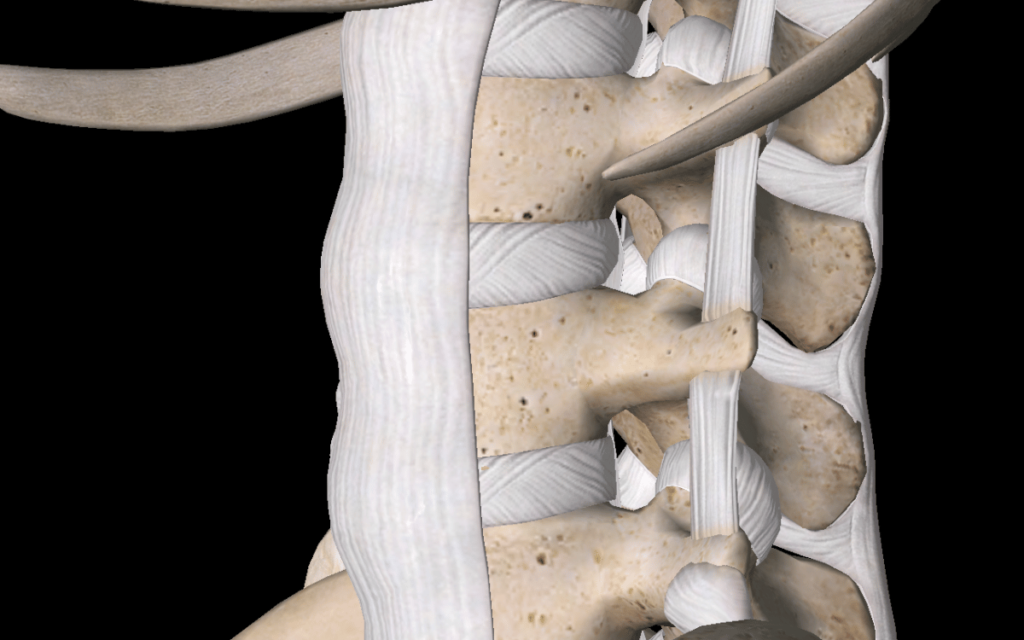
Image: Soft Tissue Structures of the Spine (3D4Medical from Elsevier, 2023)
Hernias/ruptured disc
The disc compresses and pushes out at its edges, irritating nearby nerves. This often occurs at the lumbar (lower back) level.
Spondylolysis -> Spondylolisthesis
A vertebra slips forwards, pinching on nerves that exit between adjacent vertebrae.
Spinal stenosis
Narrowing of the spinal column/canal that puts pressure on the spinal cord and exiting nerves at the ‘nerve roots’.
Fractured vertebrae
A fracture is a bone break – this ranges in severity from a hairline fracture to a bigger fracture like a spondylolisthesis.
Structural changes in your spine
Such as scoliosis, structural kyphosis, or any other changes in the spine at birth or developed over time.
(National Institute of Neurological Diseases and Stroke, 2020)
Common Triggers of Back Pain
Sitting for long periods
This puts a lot of pressure on your discs.
Bending activities
e.g. gardening, lifting heavy boxes, moving house, cleaning
Whether they are repetitive bending with a light/no load, or a single bend with a heavy load, bending activities also place a lot of pressure on your discs.
Sports
- Twisting / throwing
- Sudden reactive movements
- Quick or high load lifting/pick up
- Reaching/bending
- Poor deadlift mechanics
This can all lead to strains or sprains on your spinal ligaments/tendons or muscles, or a disc injury that pinches your nerve roots as they exit your spine.
Tight muscles/knots could also pinch on your peripheral nerves outside of your spine, such as your piriformis muscle or your hamstrings (secondary nerve pain).
Running
- High impact on your back
- Total body coordination – everything needs to know how to work together, and WELL
Pregnancy
- Sacroiliac joint (SIJ). With your ligaments becoming more lax in preparation for childbirth, this also has an impact on the supportive ligaments of your sacroiliac joint.
- Anterior pelvic tilt / increased lumbar lordosis. This can lead to strains or sprains of your spine.
- Posterior pelvic tilt / decreased lumbar lordosis. This can lead to disc problems.
- Loss of spinal articulation. This can lead to strains, sprains, disc problems.
Check out or post titled ‘Back Pain in Pregnancy: Causes, Symptoms and Treatments‘.
Disc Bulge/Hernia
One of the most common structural injuries we see are disc bulges. You’ve got two broad options for a disc bulge:
- Surgery, specifically microdiscectomy
- Conservative management by physiotherapy
Depending on the severity of your injury (usually determined by your specialist or informed by imaging findings*) and other health conditions you may have, one option may trump another. Or perhaps for you, both are fairly equal. If so, gather as much information as you can to weigh out the pros and cons of the respective options. As healthcare practitioners, don’t make the decision for you, or try to steer you toward one or the other. We just present the facts so you can make a really informed decision.
It can be said though, that many people give conservative management a good shot before deciding whether or not to go for surgery. This is especially because approximately 90% of cases are temporary, where pain improves without surgery aka with conservative management (Zalatimo, n.d.).
No matter what you decide on, it is important for a person with low back pain to continue to stay active and return to usual activity, including work, as soon as possible and as much as feasible.
We hope that doesn’t sound daunting!
To maximise function and pain-free movement so that impacts on your daily life are limited, practical and individualised self-management strategies discussed between physiotherapist and patient are critical (Australian Commission on Safety and Quality in Health Care, 2022).
Our aim is to support you through your recovery journey as physiotherapy is one of the main ways to manage back pain. We use a plethora of evidence-based techniques to help you get back to doing the things you love.
*See more under ‘Myths’.
Our Viva Framework: Relieve – Restore – Perform
- Relieve your pain
- Restore normal movement patterns
- Perform – build strength to give you a buffer to prevent further injury
Want to learn more about our approach?
Following our tried-and-tested Relieve-Restore-Perform framework, we first begin the relieve (pain) phase, by using manual therapy techniques such as massage, mobilisation of your joints or dry needling. We also teach you strategies on how to get through each day as best as possible.
As you graduate from ‘Relieve’, we move on to the ‘Restore’ phase, where we teach you progressive exercises to help your body re-learn movement patterns to move in a sustainable and functional way. Don’t worry, we start light.
‘Perform’ phase – this is where we get really strong! Many people think that once the pain is relieved, the problem is “fixed”. However, 50% of patients who suffer from episodes of low back pain will have recurrent episodes within one year (Zalatimo, n.d.). We see time and again that when people stop at ‘Relieve’ or ‘Restore’, the pain and injury returns with the smallest aggravation such as just “moving wrong” while turning to get your coffee cup from the other end of the table. 🙁
My Recommended Physio Exercises to Relieve Back Pain (and perhaps Restore healthy movement patterns)
Disclaimer: the following exercises work well with general mechanical back pain – however, for more complex issues, it’s important you see a physiotherapist to first get a diagnosis.
Pelvic tilts
- Start Position: Lay on your back, knee bent, feet flat on ground (crook-lie)
- Action: Scoop your tailbone up to the sky, pressing the small of your back into the mat. Now press your tailbone into the mat, while increasing the space between your mat and the small of your back.
- Benefit: Release tight back muscles, increase awareness and coordination of your deep core muscles.
Knee rocks
- Start Position: Crook-lie
- Action: Drop your knee to each side, starting in small ranges, and increasing the range as far as is comfortable for your body
- Benefit: Release tight back muscles
Cat cow
- Start Position: 4-point kneel, knees directly under hips, hands directly under shoulders
- Action:
– Drop your belly, shine your chest forward, poke your tailbone up
– Round your back, shoulder blades away from each other as you push into the ground, draw belly button into spine, tailbone pointing down - Benefit: Increase the ranges between each corresponding vertebrae of your spine. Increase strength of upper back muscles. Relieving stretch.
Toy soldier with a Foam roller
- Start Position: Lay on a long foam roller, right in the middle of your back. Head is rested. Knees bent and feet flat on the floor
- Action:
– Reach your arms up to shoulder height.
– Reach one arm up overhead. Return to shoulder height.
– Repeat on the other side.
– Note that you are not flaring your ribs as you reach your arms overhead. - Benefit: Improve strength and awareness of the supportive deep core muscles
Articulated shoulder bridge
- Start Position: Lie on your back with knees bent. Hands on either side of your hips.
- Action:
– Go into a few rounds of pelvic tilts to warm up.
– The next time you scoop your tailbone up, lift your tailbone off of the mat, followed by the rest of your spine, starting from lower, middle then upper back. Think of your body and mat as separating strips of velcros.
– Find neutral spine at the top of the movement
– Slowly begin to lower your body back down – starting from upper, middle, lower back and finally your tailbone.
– Find neutral spine at the bottom of the movement. - Benefit: Improve mobility of spine, strengthen glutes and supportive deep core muscles
Bird-dog
- Start Position: 4-point kneel, knees directly under hips, hands directly under shoulders. Neutral spine.
- Action:
– Simultaneously, slide one in leg back and up to hip height and reach the opposite arm up to shoulder level.
– Return to start position.
– Repeat on the other side. - Benefit: Challenges and further strengthens deep core muscles along with more global muscles, such as the gluteal/bum muscles.
Self-Relieving Strategies for Acute Aggravations/Injuries
All of the above exercises generally relieve mechanical back pain, however the following tips can be more useful for more acute injuries such as an acute disc irritation/bulge.
Again, the type of strategies and exercises for you depend highly on the type and severity of your injury. Here at Viva, our experienced physiotherapists can help you identify the best strategies for your type of pain.
Lumbar Disc Bulges
Cobra stretches in lying
- Lie face down on your bed/yoga mat.
- Place your hands under your shoulders
- Push your upper body off the bed while keeping your hips down. Stop just at the edge of restriction.
- Hold for 15-30s.
Backward stretch in standing
- Stand tall
- Place your hands on your hip bone, just above your bum.
- Push your hips forwards just to the edge of restriction.
- Hold for 15-30s.
Lumbar Facet Joint Sprains
- Child’s pose
- On a floor/bed/yoga mat: Sit on your heels, with knees bent in front of you.
- Bend forward from your hips, allow your back to curve forwards gently.
- Your hands may stay relaxed beside your hips or reaching up overhead (arms beside your ears).
- Hold for 15-30s.
Lean forward in sitting
- Sit comfortably on a chair
- Bend forward from your hips, allow your back to curve forwards gently.
- Hold for 15-30s.
Back Pain Myths
“I need to rest/lie down to relieve the pain.”
This is time-dependent! If it is an acute injury, rest lying down on your back for the first 48 hours. After the initial 48h rest period, gradually return to movement/daily activities with the guidance of your physiotherapist.
“According to my scan, I have a disc degeneration/disc bulge/herniation. I feel fine but that means I need to stop bending.”
It is important to note that scans/imaging findings are not a tell-all*.
A study summarising the findings of 33 articles (a total of 3110 people), shows that high proportions of people have imaging findings of spine degeneration/disc bulge/disc protrusion but are asymptomatic – meaning that despite scans showing a deviation from ‘normal healthy’, these people feel perfectly fine! The prevalence of these findings increased with age.
It was therefore concluded that many imaging-based degenerative features are likely part of normal ageing and unassociated with pain. Imaging findings must be interpreted in the context of your clinical presentation. It is how you present that really matters (Brinjikji et al., 2015).
When Should I Go for a Scan? Or seek further advice?
We recommend a scan if there is no improvement after 6 weeks of conservative management, or in the presence of neurological deficit such as foot drop or altered reflexes.
What happens when I “do” my back?
- Reach out to your GP or physio, they will point you in the right direction on what to do next, such as the most appropriate types of painkillers.
- First 48h is crucial for resting and lying flat
- After 48h, it is important for you to keep moving
- Visit your physio on day 3
- If your muscles are tense, you can self massage the muscles. Use a spikey ball, massage ball, or tennis ball.
Conclusion
Back pain can be debilitating, but it can get better, especially with the right support and knowledge in your toolkit. We can help you on that journey – book in to see pain physio. But also, don’t forget that when the initial pain is relieved, there is work to be done – structures to strengthen, movement patterns to correct – to reduce the high chance of reoccurrence. At Viva, we are passionate about movement (the right ones) and helping you through your road to recovery. Want to feel your best? Book an appointment.
References
American Association of Neurological Surgeons. (n.d.-a). Anatomy of the Spine and Peripheral Nervous System. Retrieved 23/12/2022 from https://www.aans.org/en/Patients/Neurosurgical-Conditions-and-Treatments/Anatomy-of-the-Spine-and-Peripheral-Nervous-System
Australian Commission on Safety and Quality in Health Care. (2022). Low Back Pain Clinical Care Standard 2022. Retrieved 22/12/2022 from https://www.safetyandquality.gov.au/sites/default/files/2022-08/low_back_pain_clinical_care_standard.pdf
Brinjikji, W., Luetmer, P. H., Comstock, B., Bresnahan, B. W., Chen, L. E., Deyo, R. A., Halabi, S., Turner, J. A., Avins, A. L., James, K., Wald, J. T., Kallmes, D. F., & Jarvik, J. G. (2015). Systematic literature review of imaging features of spinal degeneration in asymptomatic populations. AJNR. American journal of neuroradiology, 36(4), 811–816. https://doi.org/10.3174/ajnr.A4173
Hayden JA, Ellis J, Ogilvie R, Malmivaara A, van Tulder MW. Exercise therapy for chronic low back pain. Cochrane Database of Systematic Reviews 2021, Issue 9. Art. No.: CD009790. DOI: 10.1002/14651858.CD009790.pub2. Retrieved 30/01/2023.
Zalatimo, O. (n.d.). Low Back Pain. American Association of Neurological Surgeons. Retrieved 22/12/2022 from https://www.aans.org/en/Patients/Neurosurgical-Conditions-and-Treatments/Low-Back-Pain
National Institute of Neurological Diseases and Stroke. (2020). Low Back Pain Fact Sheet. Retrieved 22/12/2022 from https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Low-Back-Pain-Fact-Sheet
Frequently Asked Questions
What is the one thing you would tell people to do, to reduce the likelihood of back pain occurring?
Stay healthy, stay fit (don’t do too much at once, and don’t do too little), maintain a neutral posture (see here: for a neutral spine), look after your mental and physical health, enjoy life. Whoops that’s more than one thing – but if we take anything away from this – it would be to stay healthy, happy and balanced.
What are the best core exercises to alleviate lower back pain?
It depends on the mechanism of your lower back pain, your baseline strength, as well as the rehab phase you’re in (relieve, restore or perform).
If your LBP is a disc injury and it is quite acutely flared up, extension-type stretches would be best e.g. cobra stretches
If it is an acute facet injury or stenosis, flexion-type stretches e.g. child’s pose, forward fold, leaning forwards in a chair, would be the way to go.
If your LBP is mechanical/non-specific, or you are ready for the perform phase, there are a plethora: planks, 4 point kneel hovers, abdo prep, alternating scissors in double table-top – all while maintaining a neutral spine of course!
Still have questions? Read ‘Your Back Pain Questions Answered: A Comprehensive Guide to Understanding and Managing Back Pain.‘